Glue ear
Ninja Phoenix and DJ and The Gloopy Glop
Glue ear is a condition that affects 8 out of 10 children in the UK. We wanted to help people understand more about the condition and how it can be treated.
Glue ear is one of the most common childhood illnesses, and occurs when the middle ear becomes filled with sticky fluid. It’s usually temporary and often linked with ear infections, but long-term glue ear can affect children's hearing and speech development.
You can find more information about treating glue ear and grommets here.
What is glue ear?
Glue ear happens when the middle ear (behind the eardrum) becomes filled with sticky fluid. Otitis media with effusion (OME) is the medical name for glue ear. It’s very common – 1 in 5 pre-school children have glue ear at any one time and 8 out of 10 children will experience glue ear before the age of 10.
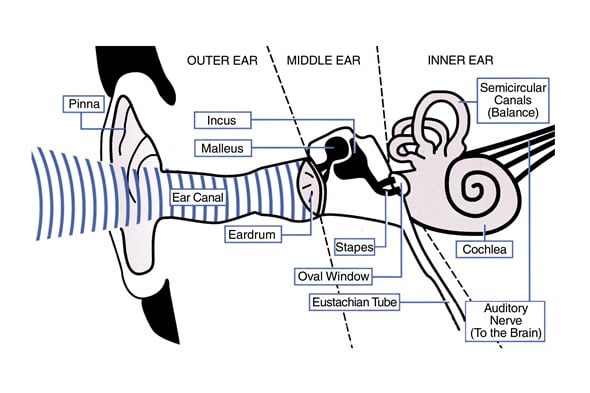
For ears to work properly the middle ear needs to be kept full of air. The air travels through the eustachian tube which runs from the middle ear to the back of the throat. In children this tube is not as vertical and wide as it will be when they get older and as a result doesn’t work as well. If the eustachian tube becomes blocked, air cannot enter the middle ear. When this happens, the cells lining the middle ear begin to produce fluid. This is a runny liquid which can get thicker as it fills the middle ear. If your child has glue ear your GP may describe their ear or ears as being ‘congested’.
With fluid blocking the middle ear, it becomes harder for sound to pass through to the inner ear, making quieter sounds difficult to hear.
Glue ear can affect one or both ears.
For more information, download our booklet Glue Ear: A guide for parents or visit the NHS website to watch a video explaining what glue ear is and how it's treated.
To chat to other parents of children experiencing glue ear, visit our glue ear group on Facebook.
What causes glue ear?
Many things can contribute to glue ear, such as colds and flu, allergies and passive smoking. It’s often but not always linked with ear infections.
Children with cleft palate, or with genetic conditions such as Down's syndrome, may be more likely to get glue ear as they often have smaller eustachian tubes that don’t function well.
Parents, Scott and Siobhan, talk to us about what it's like for their son, Bayley, to have a cleft palate, his glue ear operation and hearing loss in our video.
Does my child have glue ear?
Spot the signs of glue ear
- Changes in behaviour.
- Becoming tired.
- A lack of concentration.
- Preferring to play alone.
- Not responding when called.
These signs can often be mistaken for stubbornness, rudeness and being naughty. You could ask your child’s teacher, or other people your child has had recent close contact with, if they’ve noticed any of these signs.
Glue ear (otitis media with effusion) can cause temporary deafness and a prolonged period of time with reduced hearing can affect children’s speech and language development, for example, parts of words may not be pronounced clearly. They may also fall behind at school if they don’t have extra support.
What should I do if I think my child has glue ear?
Arrange an appointment with your GP. Often glue ear is associated with a heavy cold and will clear up when the congestion from the cold has gone.
Your GP will examine your child’s ears and should be able to tell if they have glue ear. They may describe your child’s ear or ears as ‘congested’. If there is any pain or sign of infection your GP may prescribe a course of antibiotics. It’s likely that your child won’t receive any treatment for the first three months, but they should be monitored by your GP, known as ‘watchful waiting’. If the symptoms continue your GP, health visitor or school nurse can refer you to the audiology or ear, nose and throat (ENT) department at your local hospital.
How do they test for glue ear?
An audiologist will examine your child’s ears and a further assessment will be carried out. This will include a tympanometry test, which measures how well the eardrum can move. If there is fluid in the middle ear the eardrum won’t move properly.
A graph (called a tympanogram) will show the results straight away. A hearing test should also be done to check if the glue ear is affecting your child’s hearing and by how much. These tests are very quick and are completely painless.
The audiologist should explain the results of all the tests and discuss the best way to manage your child’s symptoms. It’s a good idea to monitor the glue ear with repeated tests at least three months apart. For most children, the glue ear will clear up in this time. If it hasn’t, you may be offered grommets or temporary hearing aids.
Factors which may affect glue ear
Breastfeeding
It’s known that breast milk provides essential nutrients to help children to fight off infections in the first few months of their life. Breastfeeding also passes on the mother’s natural protection against illness. Research has shown that children who have been breastfed from birth are less likely to get glue ear at a young age. Ask your GP or health visitor for more information.
It may help to feed your baby (either breastfeeding or with a bottle) in a sitting position rather than lying flat. This helps prevent fluids entering the eustachian tube during feeding.
Smoke-free environment
Research carried out by the Department of Health has shown that all children are more likely to get ear infections and glue ear if they’re often in a smoky environment. A child is likely to experience glue ear for as long as the environment remains smoky.
Parents should try to make their children’s environment smoke-free e.g. the home and car. If it’s not possible to make the environment entirely smoke-free, then smoking should be confined to an area not used much by children. It’s important to remember that simply opening a window is not enough, as many dangerous smoke particles will stay in the air.
Allergies
Research suggests that allergy may be related to persistent glue ear in some children. You can ask your GP about testing your child for allergies or referral to an NHS allergy clinic if you think this might be the cause. Allergies to fur, pollen, dust mites or some foods may cause the eustachian tube to swell and this can prevent fluid from draining from the middle ear. For more information on allergy, you may like to contact the charity Allergy UK.
Treating glue ear
Find out more about the different treatment options for glue ear here.
How can my child's school help?
Support at school for children with glue ear
Children’s hearing can be affected for long periods of time while waiting to see if the glue ear clears up naturally or while on the waiting list to have the grommet operation or hearing aids. Some children will have glue ear for long periods that may persist through secondary school, so it’s important that your child’s speech and education doesn’t suffer.
If the glue ear persists and leads to children experiencing mild hearing loss, research shows that it can have a major impact on their development, but fortunately, there are lots of things that schools can do to support children with mild hearing loss.
As a starting point, talk to your child’s teacher or the person who has been designated by the school to identify children with special or additional educational needs to ask for extra support at school. In England, this person is known as a Special Educational Needs Coordinator (SENCO). You could also talk to a Teacher of the Deaf (ToD) from the local authority specialist education service for deaf children.
Share seven way to support a child with glue ear, from Glue Ear Together (link opens in a new tab).
The school aren’t taking my child’s glue ear seriously
Many parents of children with glue ear have told us that their child’s school doesn’t understand the impact glue ear can have on their child’s academic and speech and language development. They don’t always do enough to support children with glue ear.
England
The law (Children and Families Act 2014) requires that schools in England take steps to support children with medical conditions. Glue ear can be regarded as a ‘medical condition’. Schools must also follow government guidance called Supporting children with medical conditions. This guidance requires schools to make sure that:
- children with medical conditions are supported so that they have full access to education, including to physical education and school trips
- staff receive appropriate training
- there is someone in charge of how the school supports children with medical conditions
- they have a policy that sets out how they will support children with medical conditions (this should be readily available).
If you’re concerned about the support that your child is receiving, make sure that the school is clear that your child has a medical condition. Ask them how they’ll make sure they are meeting the requirements of the government guidance.
Wales
The Welsh Government has produced guidance for schools on children with medical conditions.
Scotland
If you live in Scotland, your child may be regarded as having ‘additional support needs’. Schools in Scotland are required to provide support for these children, even if this support is only needed for a short while. The Enquire website has more information on additional support for learning and on your rights in this area.
If your child’s glue ear is lasting for a long time and impacting on their education, they may be regarded as having special or additional educational needs. Schools and other education providers should provide special or additional educational support. Find out more about getting additional support at school.
If your child’s glue ear is likely to, or has, lasted for at least 12 months, without clearing up, then your child may be regarded as having a disability under the Equality Act. This means that schools and other education providers in England, Scotland and Wales must ensure they take steps to prevent discrimination and also proactively provide support to counter any disadvantage that your child may experience. Find out more about the Equality Act and your child’s education.
Northern Ireland
Northern Ireland has its own anti-discrimination legislation:
- The Special Educational Needs and Disability (Northern Ireland) Order 2005 (SENDO)
- The Disability Discrimination (Northern Ireland) Order 2006.
To find out more information on disability legislation in Northern Ireland call the Equality Commission for Northern Ireland on 028 90 890 890 or visit their website.
What you can do
- Explain to your child’s teacher and/or SENCO that although glue ear is usually temporary, your child is deaf and needs extra help. Show them your child’s most recent audiogram so the school understands what your child can and can’t hear.
- Seek advice from the local authority specialist education service for deaf children, who employ teams of Teachers of the Deaf (ToDs). Not all services provide direct support to children with temporary or mild hearing loss but they should provide the school with guidance and information. If your child has a hearing aid, they should have a ToD.
- Tell them about us! The National Deaf Children’s Society supports children with all types of hearing loss, including glue ear, and has lots of information for professionals who work with deaf children.
- Share our resources with your child’s teacher (and anyone else who works closely with your child) to help them understand how glue ear or mild hearing loss affects children in the classroom and what steps they can do to help make listening and learning easier.
- Encourage your child’s teacher to share our deaf awareness tips and resources with the other children so that they know how to communicate with, and include, your child.
- Explain the benefits of reducing background noise in the classroom as much as possible.
- Ensure that staff and pupils know how to communicate clearly and effectively with your child.
- Check that there has been an assessment of your child’s needs.
- Create a personal passport or profile that summarises all the most important information about your child so that school can support your child in the best way possible.
- Your child might need special educational needs (SEN) support.
If you’re still concerned that your child’s school isn’t doing enough or that your child is falling behind at school, contact our Freephone Helpline for support and guidance on what to do next.
Can my child fly with glue ear?
Generally children with glue ear (otitis media with effusion) don’t experience problems flying, although sometimes doctors don’t recommend it depending on the current condition of the ears.
The build-up of fluid in the middle ear can expand during take-off and, more commonly, landing due to changes in cabin pressure, causing discomfort. The risk is the fluid expands so much the eardrum perforates; if this happens a doctor should prescribe antibiotics but there is normally no long-term damage.
Before flying, we strongly recommend seeing your GP who may prescribe decongestant medication.
Eating and drinking during take-off and landing will help open your child’s eustachian tubes and prevent discomfort. Special ear plugs known as ‘EarPlanes’ (available from pharmacies) can help to reduce discomfort from changes in air pressure.
Hear Glue Ear app
Hear Glue Ear is an app designed for children aged two to six who are experiencing hearing loss due to glue ear. The app includes songs, games and audiobooks designed to help children to develop speech, language and listening skills and also provides information and progress-tracking for parents.
How we can help
We are here for all children and young people who are deaf or experience temporary hearing loss, including glue ear.
Join us for free to get access to one-to-one guidance from our experts, the chance to meet other families of deaf children and children experiencing glue ear, plus regular updates on the topics that are most important to you.
